.gif) VIARTIS
|
||||||||||||
|
PARKINSON'S DISEASE |
||||||||||||
|
|
||||||||||||
|
|
PARKINSON'S DISEASE NEWS
|
|
||||||||||
|
MARCH 2014 28th March 2014 - New research
COENZYME Q10 HAS NO EFFECT IN PARKINSON'S DISEASE Coenzyme Q10, an antioxidant that has been widely used for Parkinson's Disease has been found to have no significant effect. Coenzyme Q10 (CoQ10) is a supplement, which supports mitochondrial function in the neurons, and has been claimed to slow the progression of Parkinson's Disease. For more information go to Medline Plus
In previous studies Coenzyme Q10 was found to be ineffective in Parkinson's Disease in daily doses of 200mg, 300mg, 400mg, 600mg, and 800mg. Only one Coenzyme Q10 study has ever shown any improvement in Parkinson's Disease, using 360mg, but the effects were mild and were only assessed for four weeks. Daily doses of 300mg, 600mg and 1200 mg failed to improve the symptoms of Parkinson's Disease but reduced the rate of deterioration. In order to refer to this article on its own click here
23rd March 2014 - New research
PARKINSON'S DISEASE INCREASES THE RISK OF INJURIES People with Parkinson's Disease have been found to increase their likelihood of most accidental injuries, especially head injuries. The risk of injury increases with age.
The injury risk for those people with Parkinson's Disease who were 69-79 years old was significantly higher than those who were 50-69 years old. So people with Parkinson's Disease demonstrate a significantly elevated risk of developing all accidental injury types except injuries caused by burns. The risk of injury increases as age increases. In previous studies Coenzyme Q10 was found to be ineffective in Parkinson's Disease in daily doses of 200mg, 300mg, 400mg, 600mg, and 800mg. Only one Coenzyme Q10 study has ever shown any improvement in Parkinson's Disease, using 360mg, but the effects were mild and were only assessed for four weeks. Daily doses of 300mg, 600mg and 1200 mg failed to improve the symptoms of Parkinson's Disease but reduced the rate of deterioration. In order to refer to this article on its own click here.
22nd March 2014 - New research
THE EFFECT OF AGE OF ONSET ON PARKINSON'S DISEASE The clinical features and development of Parkinson's Disease has been found to differ in many respects according to the age of onset of Parkinson's Disease.
Those with young onset were found to have a more frequent family history of Parkinson's disease and longer survival. Symptoms other than tremor were more frequent as the initial symptom of the young onset group. Depression was more frequent in the young onset group than middle onset or old onset. The frequency of tremor as the first symptom increased with advancing age at onset. The frequency of treatment related dyskinesia or dystonia decreased with advancing age at onset. In order to refer to this article on its own click here.
10th March 2014 - New research
MAGNETIC RESONANCE IMAGING ACCURATELY DIAGNOSES PARKINSON'S DISEASE Parkinson's Disease has been diagnosed with almost complete accuracy using a scanning method called Magnetic Resonance Imaging (MRI).
An evaluation was carried out of the substantia nigra (SN) of people who did and who did not have Parkinson's Disease. The substantia nigra (SN) is the area of the brain most affected by Parkinson's Disease. Deviations from the normal appearance of the substantia nigra were described and indicated as abnormal. The abnormal architecture of the substantia nigra allowed a discrimination between people who did and who did not have Parkinson's Disease with a sensitivity and specificity of 100% and 96% respectively. In order to refer to this article on its own click here.
5th March 2014 - New research
L-DOPA'S EFFECT ON NON-MOTOR SYMPTOMS OF PARKINSON'S DISEASE People with Parkinson's Disease have the characteristic motor symptoms of Parkinson's Disease but also have a wide range of non-motor symptoms. Although L-dopa is a widely used basis for treating Parkinson's Disease, L-dopa (with carbidopa) has been found to have little effect on many of the non-motor symptoms of Parkinson's Disease.
Some non-motor symptoms of Parkinson's Disease are not improved by taking L-dopa because they are due to the side effects of Parkinson's Disease drugs. Some non-motor symptoms of Parkinson's Disease are not improved much by taking L-dopa because they are due to a combination of Parkinson's Disease and other factors that are not related to the dopamine deficiency that occurs in Parkinson's Disease. In order to refer to this article on its own click here.
4th March 2014 - New research
THE EFFECT OF MILD BRAIN INJURY ON PARKINSON'S DISEASE Researchers assessed all of the studies concerning the risk of Parkinson's Disease after mild traumatic brain injury. Sixty-five studies were eligible and reviewed, but only five of these with a low risk of bias were accepted as scientifically admissible.
|
||||||||||||
.gif) |
||||||||||||
| ©2006-2014 Viartis | ||||||||||||
| [email protected] | ||||||||||||
 People
with Parkinson's Disease were given either a placebo, 1200mg of CoQ10 per
day, or 2400mg of CoQ10 per day. All of them were also given 1200 IU per day
of vitamin E. Participants were observed for 16 months or until a disability
requiring dopaminergic treatment. The treatments were well tolerated with no
safety concerns. However, the worsening of Parkinson's Disease was actually
related to the higher Coenzyme Q10 dose. Those taking no Coenzyme Q10
worsened by 6.9 points on the UPDRS. Those taking 1200mg worsened by 7.5
points. Those taking 2400mg worsened by 8.0 points. So Coenzyme Q10 was not
only not beneficial it appeared, if anything, to be detrimental.
People
with Parkinson's Disease were given either a placebo, 1200mg of CoQ10 per
day, or 2400mg of CoQ10 per day. All of them were also given 1200 IU per day
of vitamin E. Participants were observed for 16 months or until a disability
requiring dopaminergic treatment. The treatments were well tolerated with no
safety concerns. However, the worsening of Parkinson's Disease was actually
related to the higher Coenzyme Q10 dose. Those taking no Coenzyme Q10
worsened by 6.9 points on the UPDRS. Those taking 1200mg worsened by 7.5
points. Those taking 2400mg worsened by 8.0 points. So Coenzyme Q10 was not
only not beneficial it appeared, if anything, to be detrimental. People
with Parkinson's Disease were found to have the following increased
likelihood of injuries times what is normal : head injury 1.9, bone fracture
and dislocation 1.4, all injuries 1.3, injury to spinal cord, plexus and
nerves 1.25, superficial injuries and contusions 1.20, burns 1.0.
People
with Parkinson's Disease were found to have the following increased
likelihood of injuries times what is normal : head injury 1.9, bone fracture
and dislocation 1.4, all injuries 1.3, injury to spinal cord, plexus and
nerves 1.25, superficial injuries and contusions 1.20, burns 1.0. 
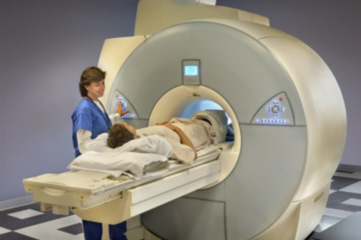 Magnetic
resonance imaging (MRI) is a type of scan that uses strong magnetic fields
and radio waves to produce detailed images of the inside of the body. An MRI
scanner is a large tube that contains powerful magnets. The patient lays
inside the tube during the scan and is moved into the scanner either head or
feet first. The MRI scanner is operated by a radiographer who controls the
scanner using a computer.
For more information go to
Magnetic
resonance imaging (MRI) is a type of scan that uses strong magnetic fields
and radio waves to produce detailed images of the inside of the body. An MRI
scanner is a large tube that contains powerful magnets. The patient lays
inside the tube during the scan and is moved into the scanner either head or
feet first. The MRI scanner is operated by a radiographer who controls the
scanner using a computer.
For more information go to
 When
assessed, the most frequent non-motor symptoms of Parkinson's Disease were
fatigue 56%, excessive sweating 54%, insomnia 54%, akathisia (restlessness)
47%, anxiety 45%, and constipation 17%. However, after five months of taking
L-dopa and carbidopa, frequencies of most of the non-motor symptoms decreased
only slightly, showing that there was little significant effect of L-dopa
and carbidopa.
When
assessed, the most frequent non-motor symptoms of Parkinson's Disease were
fatigue 56%, excessive sweating 54%, insomnia 54%, akathisia (restlessness)
47%, anxiety 45%, and constipation 17%. However, after five months of taking
L-dopa and carbidopa, frequencies of most of the non-motor symptoms decreased
only slightly, showing that there was little significant effect of L-dopa
and carbidopa.  One
of the five studies showed a significant association between Mild traumatic
brain injury and Parkinson's Disease. It was found to be 1.5 times more
likely. However, the likelihood decreased when the time between the injury
and Parkinson's Disease diagnosis was greater. The other four studies did
not find any association. So the available evidence argues against a causal
association between Mild traumatic brain injury and Parkinson's Disease.
One
of the five studies showed a significant association between Mild traumatic
brain injury and Parkinson's Disease. It was found to be 1.5 times more
likely. However, the likelihood decreased when the time between the injury
and Parkinson's Disease diagnosis was greater. The other four studies did
not find any association. So the available evidence argues against a causal
association between Mild traumatic brain injury and Parkinson's Disease.