26th January
2012 - New research
DUODENAL L-DOPA CAN CAUSE POLYNEUROPATHY
Journal of Neurology [2012] Jan 24 [Epub ahead of
print] (Santos-Garc�a D, de la Fuente-Fern�ndez R, Valldeoriola F, Palas� A,
Carrillo F, Grande M, Mir P, De Fabregues O, Casanova J.)
Complete abstract
Neurology [2011] 77 (22) : 1947-1950 (Y.A.Rajabally, J.Martey)
Complete abstract
 Reports
have emerged describing the occurrence of polyneuropathy related to vitamin B12 deficiency
and Guillain-Barr�
syndrome in people with Parkinson's Disease
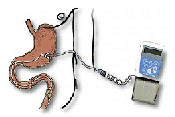
who are being treated with continuous duodenal L-dopa infusion. Duodenal L-dopa
is administered as a gel throughout the day using a portable pump directly into
the small intestine through a surgically placed tube. This ensures a flow of
L-dopa that can be adjusted according to the patient's needs. For
more information on polyneuropathy go to
Polyneuropathies.
Reports
have emerged describing the occurrence of polyneuropathy related to vitamin B12 deficiency
and Guillain-Barr�
syndrome in people with Parkinson's Disease
who are being treated with continuous duodenal L-dopa infusion. Duodenal L-dopa
is administered as a gel throughout the day using a portable pump directly into
the small intestine through a surgically placed tube. This ensures a flow of
L-dopa that can be adjusted according to the patient's needs. For
more information on polyneuropathy go to
Polyneuropathies.
At least 12 cases of polyneuropathy related to
vitamin B12 deficiency, and a
case of Guillain-Barr�
syndrome have been reported in people with
Parkinson's Disease treated with duodenal L-dopa infusion. L-dopa gel infusion
may cause a decrease in vitamin B12 levels, leading to peripheral neuropathy.
Other detrimental effects include alterations related to the metabolism of
L-dopa, abnormal L-dopa absorption, and direct neurotoxicity of L-dopa at high
doses. Vitamin B12 supplements may need to be considered in people with
Parkinson's Disease on duodenal L-dopa infusion therapy, because vitamin B12
deficiency in people on duodenal L-dopa infusion therapy may be more frequent
than the published data suggest.
In another new study, over a third (37%) of people with
Parkinson's Disease were found to have neuropathy.
Vitamin B12 deficiency was the most common cause. This could be made more likely
by the long term use of L-dopa in any form. Many people with Parkinson's Disease
who have neuropathy or Vitamin B12 deficiency are unaware of it.
In order to refer to this article on
its own
click here.
24th January 2012 - New research
DEMENTIA IS LINKED TO INSULIN RESISTANCE IN
PARKINSON'S DISEASE
Journal of Neurological Science [2012] Jan 20.
[Epub ahead of print] (Bosco D, Plastino M, Cristiano D, Colica C, Ermio
C, De Bartolo M, Mungari P, Fonte G, Consoli D, Consoli A, Fava A.) Complete abstract
Dementia has been found to be associated with insulin resistance in Parkinson's
Disease. Dementia commonly occurs in Parkinson's Disease when Parkinson's
Disease progresses. This is not inevitable because the biochemistry of
Parkinson's Disease and Dementia are completely distinct. There is therefore no
reason why they should coincide. Their common association has never been fully
explained apart from the fact that Dementia and Parkinson's Disease are both far
more common with age.
 People
who have Parkinson's Disease and dementia were assessed for their resistance to
insulin. When insulin is produced in order to prevent high blood glucose levels,
insulin sometimes does not have affect. This can be due to insulin resistance,
which is the inability of insulin to stimulate the insulin receptors. Brain
function largely requires glucose in order to function. Nearly two thirds (62%)
of people with Parkinson's Disease who had dementia were found to have insulin
resistance. 30% of them also had impaired glucose tolerance. These percentages were significantly higher when
the disease duration was longer and when the movement disability was worse. So
dementia in Parkinson's Disease appears to be affected by the inability to make
use of glucose rather than be a direct result of Parkinson's Disease.
In order to refer to this article on
its own
click here.
People
who have Parkinson's Disease and dementia were assessed for their resistance to
insulin. When insulin is produced in order to prevent high blood glucose levels,
insulin sometimes does not have affect. This can be due to insulin resistance,
which is the inability of insulin to stimulate the insulin receptors. Brain
function largely requires glucose in order to function. Nearly two thirds (62%)
of people with Parkinson's Disease who had dementia were found to have insulin
resistance. 30% of them also had impaired glucose tolerance. These percentages were significantly higher when
the disease duration was longer and when the movement disability was worse. So
dementia in Parkinson's Disease appears to be affected by the inability to make
use of glucose rather than be a direct result of Parkinson's Disease.
In order to refer to this article on
its own
click here.
14th January 2012 - New research
THE PREVALENCE OF PAIN IN PARKINSON'S DISEASE
Movement Disorders [2012] Jan 9 [Epub ahead of
print] (M.P.Broen, M.M.Braaksma, J.Patijn, W.E.Weber)
Complete abstract
Pain has been found to occur in over two thirds of
people with Parkinson's Disease. Pain has been studied more intensely as a
symptom of Parkinson's Disease in recent years. However, studies on the
characteristics and prevalence of pain in Parkinson's Disease have given
conflicting results, prompting a systematic review of the medical literature. In
the relevant studies, the frequency of pain
in Parkinson's Disease ranged from 40% to 85%
 with
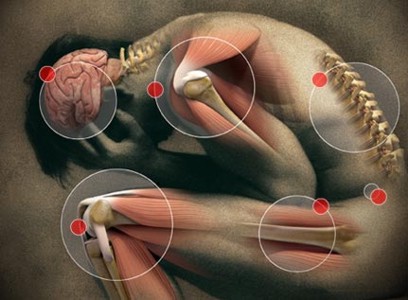
an average of 67% (just over two thirds of people). Pain in Parkinson's Disease
is most frequently located in the legs, with
almost a half (46%) of all people with Parkinson's Disease complaining about
musculoskeletal pain. The pain fluctuates
with on-off periods. A lot of the pain suffered is unrelated to the biochemistry
of Parkinson's Disease, and is therefore not due to it. Surprisingly, only just
over half (52%) of people with Parkinson's Disease with pain used
analgesics (pain killers). This means that a lot people
with Parkinson's Disease who suffer pain are going without any treatment for it. In order to refer to this article on
its own
click here.
with
an average of 67% (just over two thirds of people). Pain in Parkinson's Disease
is most frequently located in the legs, with
almost a half (46%) of all people with Parkinson's Disease complaining about
musculoskeletal pain. The pain fluctuates
with on-off periods. A lot of the pain suffered is unrelated to the biochemistry
of Parkinson's Disease, and is therefore not due to it. Surprisingly, only just
over half (52%) of people with Parkinson's Disease with pain used
analgesics (pain killers). This means that a lot people
with Parkinson's Disease who suffer pain are going without any treatment for it. In order to refer to this article on
its own
click here.
11th January 2012 - New book
PSYCHIATRY OF PARKINSON'S DISEASE
K.P.Ebmeier, J. O'Brien, J.-P. Taylor, W. F. Gattaz, W.P.Kaschka
 Publisher's
description : This book assembles short reviews from experts in the field to
chart the various psychiatric syndromes known in Parkinson's disease, their
presentation, etiology and management. Presented are special topics on
epidemiology of psychiatric symptoms, and other topics. Rarely discussed issues are
also reviewed. This publication is essential reading for old age psychiatrists,
gerontologists and neurologists who work with patients suffering from
Parkinson's disease. Health practitioners who deal with senior patients, as well
as scientists who need a quick update on the progress in this important clinical
field will find this volume a helpful reference.
Click here for more details.
For
more books concerning Parkinson's Disease go to
Parkinson's Disease Books.
In order to refer to this article on its own
click here.
Publisher's
description : This book assembles short reviews from experts in the field to
chart the various psychiatric syndromes known in Parkinson's disease, their
presentation, etiology and management. Presented are special topics on
epidemiology of psychiatric symptoms, and other topics. Rarely discussed issues are
also reviewed. This publication is essential reading for old age psychiatrists,
gerontologists and neurologists who work with patients suffering from
Parkinson's disease. Health practitioners who deal with senior patients, as well
as scientists who need a quick update on the progress in this important clinical
field will find this volume a helpful reference.
Click here for more details.
For
more books concerning Parkinson's Disease go to
Parkinson's Disease Books.
In order to refer to this article on its own
click here.
7th January 2012 - New research
URINARY DYSFUNCTION IN PARKINSON'S DISEASE
Journal of Neurological and Neurosurgical Psychiatry [2011] 82 (12) : 1382-1386
(T.Uchiyama, R.Sakakibara, T.Yamamoto, T.Ito, C.Yamaguchi, Y.Awa, M.Yanagisawa,
Y.Higuchi, Y.Sato, T.Ichikawa, T.Yamanishi, T.Hattori, S.Kuwabara)
Complete abstract
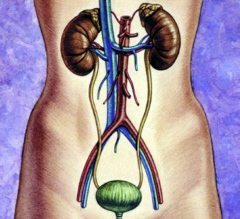 Urinary
dysfunction is common in Parkinson's Disease, but little is known about urinary
dysfunction in early and untreated Parkinson's Disease. Nearly two thirds (64%)
of people with Parkinson's Disease complain of urinary symptoms. However, there
were found to be actual urinary problems in 85% of people with Parkinson's
Disease. All of the 64% of people complaining of urinary symptoms had difficulty
controlling the retention of urine, or lost control of urinary retention
(storage abnormalities). Over a quarter (28%) had difficulty in urinating. Over half (58%) had detrusor overactivity. The
detrusor muscle is the muscle that contracts when urinating to squeeze out
urine. However, whilst urinating, detrusor
underactivity rather than overactivity occurred in half of people.
Urinary
dysfunction is common in Parkinson's Disease, but little is known about urinary
dysfunction in early and untreated Parkinson's Disease. Nearly two thirds (64%)
of people with Parkinson's Disease complain of urinary symptoms. However, there
were found to be actual urinary problems in 85% of people with Parkinson's
Disease. All of the 64% of people complaining of urinary symptoms had difficulty
controlling the retention of urine, or lost control of urinary retention
(storage abnormalities). Over a quarter (28%) had difficulty in urinating. Over half (58%) had detrusor overactivity. The
detrusor muscle is the muscle that contracts when urinating to squeeze out
urine. However, whilst urinating, detrusor
underactivity rather than overactivity occurred in half of people.
These urinary symptoms were not correlated with gender, severity of Parkinson's
Disease, or the type of motor symptom. Urinary dysfunction, manifested primarily
as storage abnormalities, and with subclinical voiding difficulties commonly
occurs in early and untreated Parkinson's Disease. For more
information concerning urinary function go to
Urinary System. In order to refer to this article on
its own
click here.
7th January 2012 - New book
DEEP BRAIN STIMULATION
Kelvin L. Chou, Susan Grube, Parag Patil
 Publisher's
description : Deep brain stimulation has dramatically changed the lives of many
patients with uncontrollable tremors. Patients often can resume normal
activities, such as feeding and dressing themselves. The need for anti-tremor
medications is often reduced or eliminated. Though it's no longer considered
experimental, DBS is, for now, still used as a second- or third-line treatment,
reserved for patients with more advanced cases of the disease and those for whom
medication alone is inadequate or can't be adjusted precisely enough to keep
their tremors and writhing under control. Deep Brain Stimulation is the first
book to be written by a team of experts that clearly explains the benefits,
pros, and cons of this revolutionary new treatment.
Click here for more details.
For
more books concerning Parkinson's Disease go to
Parkinson's Disease Books.
Publisher's
description : Deep brain stimulation has dramatically changed the lives of many
patients with uncontrollable tremors. Patients often can resume normal
activities, such as feeding and dressing themselves. The need for anti-tremor
medications is often reduced or eliminated. Though it's no longer considered
experimental, DBS is, for now, still used as a second- or third-line treatment,
reserved for patients with more advanced cases of the disease and those for whom
medication alone is inadequate or can't be adjusted precisely enough to keep
their tremors and writhing under control. Deep Brain Stimulation is the first
book to be written by a team of experts that clearly explains the benefits,
pros, and cons of this revolutionary new treatment.
Click here for more details.
For
more books concerning Parkinson's Disease go to
Parkinson's Disease Books.
.gif)
.gif)
 Reports
have emerged describing the occurrence of polyneuropathy related to vitamin B12 deficiency
and Guillain-Barr�
syndrome in people with Parkinson's Disease
who are being treated with continuous duodenal L-dopa infusion. Duodenal L-dopa
is administered as a gel throughout the day using a portable pump directly into
the small intestine through a surgically placed tube. This ensures a flow of
L-dopa that can be adjusted according to the patient's needs. For
more information on polyneuropathy go to
Reports
have emerged describing the occurrence of polyneuropathy related to vitamin B12 deficiency
and Guillain-Barr�
syndrome in people with Parkinson's Disease
who are being treated with continuous duodenal L-dopa infusion. Duodenal L-dopa
is administered as a gel throughout the day using a portable pump directly into
the small intestine through a surgically placed tube. This ensures a flow of
L-dopa that can be adjusted according to the patient's needs. For
more information on polyneuropathy go to
 People
who have Parkinson's Disease and dementia were assessed for their resistance to
insulin. When insulin is produced in order to prevent high blood glucose levels,
insulin sometimes does not have affect. This can be due to insulin resistance,
which is the inability of insulin to stimulate the insulin receptors. Brain
function largely requires glucose in order to function. Nearly two thirds (62%)
of people with Parkinson's Disease who had dementia were found to have insulin
resistance. 30% of them also had impaired glucose tolerance. These percentages were significantly higher when
the disease duration was longer and when the movement disability was worse. So
dementia in Parkinson's Disease appears to be affected by the inability to make
use of glucose rather than be a direct result of Parkinson's Disease.
In order to refer to this article on
its own
People
who have Parkinson's Disease and dementia were assessed for their resistance to
insulin. When insulin is produced in order to prevent high blood glucose levels,
insulin sometimes does not have affect. This can be due to insulin resistance,
which is the inability of insulin to stimulate the insulin receptors. Brain
function largely requires glucose in order to function. Nearly two thirds (62%)
of people with Parkinson's Disease who had dementia were found to have insulin
resistance. 30% of them also had impaired glucose tolerance. These percentages were significantly higher when
the disease duration was longer and when the movement disability was worse. So
dementia in Parkinson's Disease appears to be affected by the inability to make
use of glucose rather than be a direct result of Parkinson's Disease.
In order to refer to this article on
its own  with
an average of 67% (just over two thirds of people). Pain in Parkinson's Disease
is most frequently located in the legs, with
almost a half (46%) of all people with Parkinson's Disease complaining about
musculoskeletal pain. The pain fluctuates
with on-off periods. A lot of the pain suffered is unrelated to the biochemistry
of Parkinson's Disease, and is therefore not due to it. Surprisingly, only just
over half (52%) of people with Parkinson's Disease with pain used
analgesics (pain killers). This means that a lot people
with Parkinson's Disease who suffer pain are going without any treatment for it. In order to refer to this article on
its own
with
an average of 67% (just over two thirds of people). Pain in Parkinson's Disease
is most frequently located in the legs, with
almost a half (46%) of all people with Parkinson's Disease complaining about
musculoskeletal pain. The pain fluctuates
with on-off periods. A lot of the pain suffered is unrelated to the biochemistry
of Parkinson's Disease, and is therefore not due to it. Surprisingly, only just
over half (52%) of people with Parkinson's Disease with pain used
analgesics (pain killers). This means that a lot people
with Parkinson's Disease who suffer pain are going without any treatment for it. In order to refer to this article on
its own  Publisher's
description : This book assembles short reviews from experts in the field to
chart the various psychiatric syndromes known in Parkinson's disease, their
presentation, etiology and management. Presented are special topics on
epidemiology of psychiatric symptoms, and other topics. Rarely discussed issues are
also reviewed. This publication is essential reading for old age psychiatrists,
gerontologists and neurologists who work with patients suffering from
Parkinson's disease. Health practitioners who deal with senior patients, as well
as scientists who need a quick update on the progress in this important clinical
field will find this volume a helpful reference.
Publisher's
description : This book assembles short reviews from experts in the field to
chart the various psychiatric syndromes known in Parkinson's disease, their
presentation, etiology and management. Presented are special topics on
epidemiology of psychiatric symptoms, and other topics. Rarely discussed issues are
also reviewed. This publication is essential reading for old age psychiatrists,
gerontologists and neurologists who work with patients suffering from
Parkinson's disease. Health practitioners who deal with senior patients, as well
as scientists who need a quick update on the progress in this important clinical
field will find this volume a helpful reference.
 Urinary
dysfunction is common in Parkinson's Disease, but little is known about urinary
dysfunction in early and untreated Parkinson's Disease. Nearly two thirds (64%)
of people with Parkinson's Disease complain of urinary symptoms. However, there
were found to be actual urinary problems in 85% of people with Parkinson's
Disease. All of the 64% of people complaining of urinary symptoms had difficulty
controlling the retention of urine, or lost control of urinary retention
(storage abnormalities). Over a quarter (28%) had difficulty in urinating. Over half (58%) had detrusor overactivity. The
detrusor muscle is the muscle that contracts when urinating to squeeze out
urine. However, whilst urinating, detrusor
underactivity rather than overactivity occurred in half of people.
Urinary
dysfunction is common in Parkinson's Disease, but little is known about urinary
dysfunction in early and untreated Parkinson's Disease. Nearly two thirds (64%)
of people with Parkinson's Disease complain of urinary symptoms. However, there
were found to be actual urinary problems in 85% of people with Parkinson's
Disease. All of the 64% of people complaining of urinary symptoms had difficulty
controlling the retention of urine, or lost control of urinary retention
(storage abnormalities). Over a quarter (28%) had difficulty in urinating. Over half (58%) had detrusor overactivity. The
detrusor muscle is the muscle that contracts when urinating to squeeze out
urine. However, whilst urinating, detrusor
underactivity rather than overactivity occurred in half of people.
 Publisher's
description : Deep brain stimulation has dramatically changed the lives of many
patients with uncontrollable tremors. Patients often can resume normal
activities, such as feeding and dressing themselves. The need for anti-tremor
medications is often reduced or eliminated. Though it's no longer considered
experimental, DBS is, for now, still used as a second- or third-line treatment,
reserved for patients with more advanced cases of the disease and those for whom
medication alone is inadequate or can't be adjusted precisely enough to keep
their tremors and writhing under control. Deep Brain Stimulation is the first
book to be written by a team of experts that clearly explains the benefits,
pros, and cons of this revolutionary new treatment.
Publisher's
description : Deep brain stimulation has dramatically changed the lives of many
patients with uncontrollable tremors. Patients often can resume normal
activities, such as feeding and dressing themselves. The need for anti-tremor
medications is often reduced or eliminated. Though it's no longer considered
experimental, DBS is, for now, still used as a second- or third-line treatment,
reserved for patients with more advanced cases of the disease and those for whom
medication alone is inadequate or can't be adjusted precisely enough to keep
their tremors and writhing under control. Deep Brain Stimulation is the first
book to be written by a team of experts that clearly explains the benefits,
pros, and cons of this revolutionary new treatment.